
Physician moral injury – not burnout
“Front-line”, “battle”, “the trenches”. These terms are all too familiar when talking about modern medicine. Why are we referencing war when we should be talking about healing?

“Front-line”, “battle”, “the trenches”. These terms are all too familiar when talking about modern medicine. Why are we referencing war when we should be talking about healing?

The Japanese concept of Wabi Sabi beautifully captures the essence of life: appreciating the imperfect, the impermanent, and the incomplete. It reminds us to cherish the journey, with all its ups and downs – especially in medicine – instead of obsessing over destinations or goals.

Physician burnout is not a result of individual physician characteristics, but is significantly influenced by systemic factors within the healthcare system. In this blog, we will delve into the concept that physician burnout is more accurately described as an administrative or systemic disorder rather than an individual problem disorder, emphasizing the organizational, cultural, and economic factors that contribute to burnout in doctors.

In Part 2 of this series, we will look at further at the etiology of physician burnout, specifically the roles of medical training and leadership.

The epidemic of burnout among physicians and other healthcare professionals is here and it ain’t going away (yet). This article explores the key underlying causes of physician burnout and moral injury.

Physician Poetry: How To Be a Good Doctor On a Very Bad Day. The writer beautifully articulates the quiet suffering so many of us endure—the shame, the imposter syndrome of self-doubt, and the silent suffering and unnecessary isolation that comes with the weight of our responsibilities and our toxic medical system.

Physicians are sick, and it’s getting worse. Yet too few doctors seek help or reach out when we are struggling. Record numbers of us are burning out, becoming mentally ill or addicted, retiring early, and leaving medicine.
In this article, Part 2, I concede that there are some excellent principles differentiating ineffective from effective physician resilience programs. We hope that colleagues and medical leaders designing such programs will find the guidance useful, and further grasp the nettle of addressing the root causes of physician burnout.

Resilience programs, springing up like mushrooms, are a sticking plaster to avoid dealing with the fungating tumor underneath. We have to talk openly about the demands of modern medicine and how these are hurting the healers we need the most.

Practicing medicine is making us physicians sick. Physicians in the US have some of the highest burnout, mental illness, addiction, and suicide rates in the world. Medical student and physician burnout and suicide are a “silent epidemic”.

Modern medicine is no stranger to the toxic trio of burnout, stress, and dissatisfaction, and perfectionism plays the role of the puppet master. It’s time to swap the scalpel for a mirror and reflect. Bowlby’s framework challenges physicians to redefine excellence, shifting from unattainable perfection to a sustainable “good enough” approach.

My biggest fear in medicine is messing up. Inevitably, it happens. And while we rightly are trained to reflect, detect and learn from errors, improve practice, and ultimately save lives, the flip side – the cost of excessive perfectionism – can be very high, especially on physician well-being.

Behind the crisp white coats and stethoscopes, there lies a silent majority—physicians who are silently suffering from the immense pressures of their profession — and barriers to help.
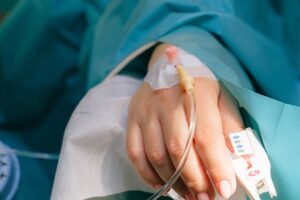
In Part 2, guest writer Dr Bryce Bowers has to move from losing a young patient under tragic circumstances onto another young patient without a moment to breathe.

“Trauma 1!” I heard them yell. “Let’s go! Let’s go!”
I stood. Frozen. Trying to process all that was going on.
Then I felt a large palm on the upper part of my back.
“Come on, kid. It’s your time to shine”.

The demanding nature of modern medicine places physicians under significant stress and strain, prompting a growing interest in the benefits of therapy to help them navigate the complexities of their profession. Engaging in proactive therapy can offer physicians a unique opportunity to enhance their insight, manage stress, and foster emotional well-being. However, like any intervention, it comes with its own set of advantages and disadvantages.
“Physician heal thyself,” says the aphorism. By extension, we could also say, “Physician know thyself”. Understanding one’s priorities is a crucial aspect of personal development. Here are five self-help exercises, including the obituary/eulogy exercise, to help individuals gain clarity on their priorities:

So the new year is near, and physicians everywhere are planning to make 2024 an even better one. Our intentions may be to engage in more self-care, develop a better LIFE-work-balance, and learn about ourselves in an “examined life”. In this context, the debate between therapy and coaching for physicians takes center stage, raising important questions about the most suitable approach for addressing the unique challenges faced by medical professionals.

As a trained psychiatrist, workaholic, depressive, and (formerly) excellent clinician, I’ve come to the following maxim with apologies to REM: “Everybody needs a little therapy (sometimes)”. As the year winds down and the nights draw in, we are taking time to reflect on 2023. Over the next weeks over the Holidays and after we ring in the new year, Physicians Anonymous will be publishing a series on self-examination.

We’ve achieved a TON in 2023, especially as we are self-funded and run by volunteers. So from 2024- HOW do we reach the suffering physician? How do we let our colleagues know that there is a safe place where they can be human first, healer second? Where they will not be judged, but they will be heard and loved. Where we can laugh and cry together bonded by the commonality of being wounded healers.

Unlike overt resignations, quiet quitting manifests as a subtle withdrawal, marked by disengagement and diminished job satisfaction. To effectively address this issue, it is imperative to delve into the scale of the problem, understand the causes behind this quiet exodus, and propose actionable solutions tailored to mitigate its impact.